Why Do Diabetics Feet Turn Black? (How To Avoid)
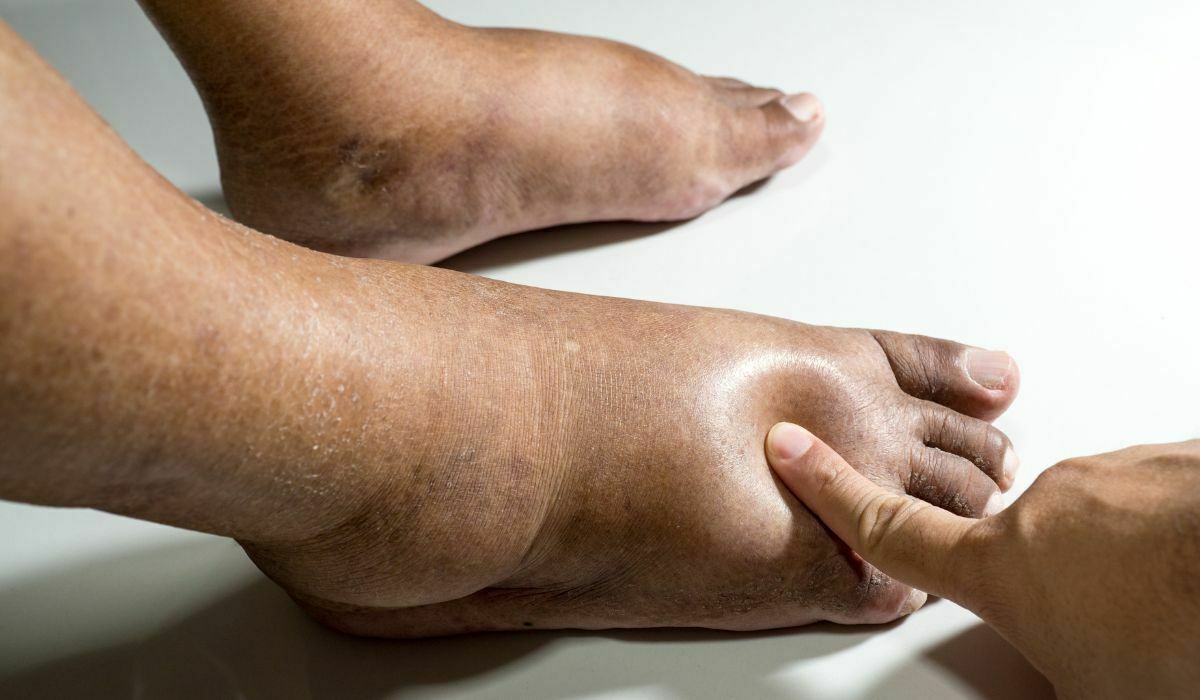
Some diabetics are known to have foot issues and circulation problems, some of which can start to become a serious health problem. Why is it that some individuals with diabetes end up with black feet?
Diabetic feet turn black when a skin injury such as a blister or sore go untreated or undetected for too long in the presence of poor circulation. This condition, known as gangrene, is very serious. Gangrene can lead to life-threatening complications, which sometimes results with amputation of a limb.
Diabetes can affect all parts of the body, including the skin. Changes in skin health can often be one of the first signs of diabetes. Diabetic skin injuries, like blisters, sores, and cuts are commonly found on the legs and feet.
When neglected, these wounds can quickly become infected and lead to complications, one being gangrene. While this may be alarming, there are several preventative measures you can take to avoid a foot wound from being a major health problem.
What is gangrene?
Gangrene is often the result of an injury or infection of the skin and soft tissue. Disrupted blood flow to the affected area can lead to the death of body tissues. Gangrene typically affects the toes, fingers, and limbs, and less commonly the muscles and organs. It is generally characterized by a discoloration of the skin, feelings of numbness, and the formation of discharge or pus.

Who is at risk?
If you have diabetes, you have an increased risk of developing gangrene. Hyperglycemia (high blood sugar levels) can cause damage to your nerves, leading to a loss of sensation in the affected area, known as diabetic neuropathy. This condition makes it easier for you to develop an injury that may go undetected.
High blood pressure is another factor that increases your risk of developing gangrene. The resistance of blood flow caused by blood vessel constriction causes a chain reaction.
If you experience poor circulation in your lower extremities due to high blood pressure, fewer infection-fighting cells can make their way to your feet, making it more difficult to heal any wounds you may develop in that area and potentially leading to infection.
People with diabetes are at particularly high risk of gangrene because of other symptoms caused by diabetes, including:
- Nerve damage or poor blood flow in the feet
- Uncontrolled blood glucose levels over long periods, including frequent episodes of hyperglycemia
- A BMI (Body Mass Index) of more than 25 (overweight/obesity)
- Hypertension (high blood pressure)
- Hyperlipidemia (high cholesterol)
Other risk factors
Individuals with underlying medical conditions that affect proper circulation are at the most risk of developing gangrene. In addition to diabetes, other conditions that affect the blood vessels and can increase your risk include:
- Peripheral arterial disease (PAD)
- Atherosclerosis
- Raynaud’s phenomenon
Having recent surgery or experiencing a traumatic injury can also increase your risk of developing gangrene.
Types of gangrene
Not all cases of gangrene are the same. It is important to understand the different types of gangrene, potential causes, and unique characteristics so proper treatment can be given.
Dry Gangrene: Associated with lack of blow flow and oxygen to affected areas. Lack of oxygen through blood leads to the deterioration of tissues and tissue death. Characterized by dry and wrinkled skin that is dark green, purple, or almost black in color.
Wet Gangrene: Develops after experiencing a minor toe or foot injury. Lack of ability to heal and decreased blood flow may result in infection. Characterized by a “wet” appearance in addition to blisters and swelling.
Gas Gangrene: Typically appears after severe trauma or a recent surgery. The development of harmful bacteria releases gas in the skin, causing tissue, cell, and blood vessel damage. Skin appears “bubbly,” swollen, and has a brownish-red color.
Signs & symptoms
It is important to recognize the early warning signs of foot problems to prevent further complications. Look for the following signs and symptoms:

- Burning, tingling, or painful feet
- Loss of sensation to heat, cold, or touch
- Changes to the color or shape of your feet
- Loss of hair on the toes, feet, and lower legs
- Thickening and yellowing of toenails
- The onset of red spots, blisters, sores, ulcers, infected corns, or ingrown toenails
- A cut, blister, or bruise that does not start to heal in a few days
- A callus with dried blood inside
- An infection that becomes black and smells bad could potentially be gangrene
Serious foot problems can develop quickly. If you notice any of the above symptoms, it is recommended to contact your health provider as soon as possible.
How are diabetes-related foot conditions diagnosed?
Your healthcare provider will do the following to help diagnose diabetes-related foot conditions:
- Ask about your symptoms and how well you’re managing blood glucose
- Perform a physical examination of your toes, feet, and leg for any signs of infection, including redness, swelling warmth, discoloration, or discharge
- Use various tools to check whether you have numbness
- Order tests, such as X-ray or MRI
- Take a sample of the skin or discharge to test for infection
Treatment
If you have diabetes and notice a foot wound, it’s important to treat the area immediately. For less severe foot wounds, treatment may include:
- Cleaning the wound
- Draining any fluid or pus from the sore or ulcer
- Apply special bandages and ointments to absorb excess fluid, protect and help heal the wound
- Prescribing a wheelchair, crutches, or medical boot to take the weight off of the affected foot
Commonly with gangrene, it is necessary to remove the infected tissue as soon as possible to prevent it from spreading to other parts of the body. This medical procedure is performed by your doctor and is called a debridement.
Furthermore, your doctor may also recommend a skin graft. A skin graft is a form of reconstructive surgery to help repair the damaged skin and any defects left after the debridement.
Healthy skin is removed from a different area of the body unaffected by gangrene and used to replace the damaged skin.
Depending on how severe the infection is, your healthcare provider may recommend hospitalization and for the area with gangrene to be removed or amputated, followed by a course of antibiotics to fight off any infection.
How to prevent gangrene
Controlling your blood sugar levels and taking proper care of your feet daily are the best steps to preventing serious diabetic foot problems, like gangrene. You can also take extra precautions and reduce your risk of diabetes-related foot conditions by doing the following:
- Monitoring your weight. Being overweight or obese can increase stress on your arteries, causing blood flow to restrict and leading to an increased risk of infection of wounds.
- Dress for the elements. Stay bundled up and warm during cold weather, as frostbitten skin can lead to gangrene. If you are experiencing abnormally pale, cold, or numb skin after being exposed to the cold, you should seek medical attention immediately.
- Quit smoking. Long-term use of tobacco weakens blood vessels and can increase your risk of developing gangrene.
How can I protect my feet if I have diabetes?
Again, the best way to protect your feet is by monitoring and controlling your blood sugar levels every day. This will help keep nerve and blood vessel damage from worsening. The next step is to keep the skin of your feet healthy.

Foot care for people with diabetes:
- Check your feet daily. Look for cuts, redness, and other changes in the skin.
- Wash your feet every day. Use warm water and soap. Do not soak your feet, it can lead to dry skin.
- Dry your feet. Infections tend to develop in moist areas. After washing your feet, Pat them dry, especially between your toes.
- Moisturize dry skin. If the skin on your feet feels rough or dry, use lotion or oil to moisturize. Do not use lotion between your toes.
- Ask your doctor to remove corns and calluses safely. Thick skin on your feet can rub and lead to sores.
- Trim your toenails straight across with a clipper. If it’s hard for you to trim your toenails, have a podiatrist (foot doctor) do it for you.
- Always wearing well-fitting shoes, socks, or slippers to protect your feet when walking. You don’t want to walk barefoot, even indoors. And be sure your shoes are smooth inside to prevent raw skin from rubbing against seams or pebbles.
- Protect your feet from heat and cold. Use sunscreen on exposed skin and don’t walk barefoot at the beach. In cold weather, wear warm socks instead of warming your feet near a heater or fireplace.
- Keep the blood flowing in your feet. Put your feet up when you’re sitting. Wiggle your toes and get plenty of activity, like walking. Avoid wearing tight socks.
- Get your feet checked at your health care visits. Even if you haven’t noticed a problem, it’s recommended to have your healthcare provider examine your feet at least once a year.
It is equally as important to avoid certain things. Avoid doing the following:
- Cutting calluses or corns or applying chemicals to the affected area yourself
- Soaking your feet
- Walking around barefoot
- Wearing tight socks or shoes
Conclusion
Although you may be at higher risk of developing gangrene and other diabetes-related foot injuries, most skin conditions can, fortunately, be prevented and easily treated if caught early enough. Although some foot conditions may simply be a cosmetic issue and harmless, you should always keep an eye out for any changes in the skin that may indicate an infection is forming. Talk to your medical provider about any concerns you may have, as it is always better to be safe, even if it may appear to be minor.
Resources
Diabetic Dermopathy Condition, Treatments and Pictures for Adults – Skinsight
Diabetes-Related Foot Conditions: Symptoms, Causes, Treatment & Prevention (clevelandclinic.org)
Gangrene and Diabetes: Understanding the Link (healthline.com)

Thanks for stopping by my Dealing With Diabetes blog! My name is LeeAnna.